The Nervous System: Words to Know
|
The Human Nervous System
- Human Neurology
The nervous system is essentially a biological
information highway, and is responsible for
controlling all the biological processes and
movement in the body, and can also receive
information and interpret it via electrical
signals which are used in this nervous system
It consists of the Central Nervous System (CNS), essentially the processing area and the Peripheral Nervous System which detects and sends electrical impulses that are used in the nervous system The Central Nervous System (CNS)The Central Nervous System is effectively the centre of the nervous system, the part of it that processes the information received from the peripheral nervous system. The CNS consists of the brain and spinal cord. It is responsible for receiving and interpreting signals from the peripheral nervous system and also sends out signals to it, either consciously or unconsciously. This information highway called the nervous system consists of many nerve cells, also known as neurones, as seen below. The Nerve Cell
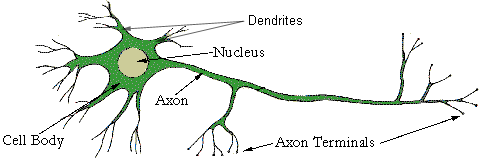
Each neurone consists of a nucleus situated in the cell body, where outgrowths called processes originate from. The main one of these processes is the axon, which is responsible for carrying outgoing messages from the cell. This axon can originate from the CNS and extend all the way to the body's extremities, effectively providing a highway for messages to go to and from the CNS to these body extremities. Dendrites are smaller secondary processes that grow from the cell body and axon. On the end of these dendrites lie the axon terminals, which 'plug' into a cell where the electrical signal from a nerve cell to the target cell can be made. This 'plug' (the axon terminal) connects into a receptor on the target cell and can transmit information between cells The Way Nerve Cells CommunicateThe "All-Or-None-Law" applies to nerve cell communication as they use an on / off signal (like an digital signal) so that the message can remain clear and effective from its travel from the CNS to the target cell or vice versa. This is a factor because just like electricity signals, the signal fades out and must be boosted along its journey. But if the message is either 1 or 0 (i.e.) on or off the messages are absolute. Classification of NeuronesInterneurones - Neurones
lying entirely within the CNS The next page elaborates on how the nervous system works... |
The Conscious & Unconscious Nervous System
- Human Neurology
The Central Nervous System is arguably the most
important part of the body because of the way it
controls the biological processes of our body
and all conscious thought. Due to their
importance, they are safely encased within
bones, namely the cranium protecting the brain
and the spine protecting the spinal cord
Brain DivisionsThere are three main components of the brain, namely the brainstem, cerebellum and the forebrain. These are elaborated upon below
The ForebrainThe forebrain has many activities that it is responsible for and is divided into many component parts. The below list elaborates on the localised areas of the forebrain and their functions.
The above components of the brain work in tandem in a healthy brain. However, in some cases the brain can be injured in some way, causing brain damage. The next page looks at how brain damage can affect the way we operate. |
The Central Nervous System
- Human Neurology
Myelin SheathMyelin is a substance that forms the myelin sheath associated with nerve cells. This sheath is a layer of phospholipids that increases the conductivity of the electrical messages that are sent through the cell. Diseases such as multiple sclerosis are a result in a lack of this myelin sheath, with the resultant effect being that the conductivity of signals is much slower severely decreasing the effectiveness of the nervous system in sufferers. In total, there are 43 main nerves that branch of the CNS to the peripheral nervous system (the peripheral system is the nervous system outside the CNS. These are the efferent neurones that carry signals away from the CNS to the peripheral system. Somatic Nervous SystemThese efferent fibres are divided into the somatic nervous system and the autonomic nervous system. The somatic fibres are responsible for the voluntary movement of our body, i.e. movement that you consciously thought about doing. The Autonomic Nervous SystemThe autonomic nervous system incorporates all the impulses that are done involuntarily, and are usually associated with essential functions such as breathing, heartbeat etc. However this type of system can further be broken down into the sympathetic and parasympathetic systems which keep one another in check in a form of negative feedback such as the release of insulin and glucagon in sugar control of the blood. All of the actions executed by the autonomic nervous system are unconsciously done. These informational pulses executed in our nervous system allow us to do our daily functions. The processing of this information is done in the CNS, the brain, a highly developed mass of nerve cells. The inner workings of the brain are investigated on the next page. |
Types and Causes of Brain Damage
- Human Neurology
Causes of Brain DamageThe brain is a highly specialised tissue, far more complex than today's 21st century supercomputers. Due to this magnificent complexity, even the slightest damage can have extreme consequences The brain can be damaged in a variety of ways, and depending on the areas damaged and the severity of the damage, it can prove relatively harmless to fatal. Some causes of brain damage are below
Types of Brain Damage
The next page of this neurology tutorial takes a further look at the brain, and the capabilities of it to be used to our advantage in daily life. |
IQ, Creativity and Learning
- Human Neurology
Evolution of Human IntelligenceHuman's, as evolved as we are, are the species most capable of exhibiting intelligence and creativity due to our capacity to learn. It is nothing short of remarkable how we, intelligent beings, came to exist.
In light of this snowball effect, and as a continuation of the last bulleted point; we have been able to sustain a rising human population over time. In turn, in accordance with natural selection, more intelligent people may be favoured by our gene pool over the long term, thus making the species as a whole more intelligent as a collective. Ability to LearnHumans continually learn from one another and share their information over generations. This is what makes our species a cut above the rest. Our ability to understand the value of learning and to do so gives us the tool to understand more and more about ourselves and our environment. IntelligenceIntelligence offers us the means to utilise abstract ideas and implement reasoning in our arguments to justify the things we do. The degree of intelligence in people is variable to a number of factors, like genetics, the local environment and even diet. It is important to note the following
CreativityIt does not take an intelligent person to be creative. It is a popular belief that technically minded people tend to be less creative as others, who, in turn, are not very technically minded. It is believed that creativity is made possible in the right brain hemisphere while the technical information is processed in the left hemisphere. It is worth noting that many of the famous creative individuals, all the famous writers, artists etc were generally intelligent. Creativity can rely on a number of factors, some of which are named below
Moreover to the last factor, it is worth considering that any factor in the external environment will be a factor in your creativity. If someone offered you a million euros to write a good poem, you may instantaneously feel more creative! Moving one step on from the conscious learning mind, we look at the unconscious mind on the next page; via sleep and dreams. |
Sleep and Dreams - Neurology
- Human Neurology
The Falling Asleep ProcessDuring the day when we are a awake, our body and brain are working tirelessly to operate our body, and as they do so they slowly degrade at a cellular level. A person will get progressively tired from this bodily breakdown, because sleep gives us a chance to build and replace the cells and resolve our end of day homeostatic imbalances. If you have not slept for a while, the decrease in the efficiency and effectiveness of the body begins to tell, and you will begin to feel sleepy as less energy is available to you. The longer we stay up the more likely we will fall asleep. If certain conditions prevail, like a state of inactivity or relaxing in a warm dry place, there is a higher chance of us falling asleep due to the preferable conditions for us to do so. SleepingWhen we fall asleep, our metabolic rate slows down, as does almost every other function across the board, we effectively go into hibernation mode. The amount of adrenaline in our body promoting awareness decreases and somatotrophin, controlling the repair of tissue is more abundant. This is effectively the healing process of sleep that revitalises us. The synaptic nerve connections containing recollections about the last day are also strengthened, hence when you wake up the more you realised you did yesterday. This localised area of memory is what many of our dreams consist of, our past recollections of the day. You may have dreamt something twice, and on the second time it was only because you thought of that first dream the day before you dreamt the second. When looking at it like this, it confirms the reason why you have the same dream, your conscious thought about it accesses that part of the brain thus 'remembers' it at night. Dreams Telling the Future?Some people believe that dreams tell the future. But, when 6 billion people dream every night, there is bound to be a coincidence when there are trillions of dreams every year. Those people who have dreamed of winning the lottery are one of many. I, personally don't believe they tell the future, though could be a sign of intelligence, the brain interpreting possibilities in the future from the knowledge of past events. This would be perfectly viable, as it would be a case of the brain 'adapting' to its future environment, and preparing you for the possible future. REMREM stands for rapid eye movement and is the points in time during sleep where dreams occur. They occur after periods of deep sleep. As suggested, rapid eye movement occurs in REM, while the body is under a state of paralysis. In effect, our brain takes us on a virtual reality of our thoughts while it steadily repairs itself for the next day. The most vivid and deepest dreams will occur in the periods between REM while drowsy, almost conscious dreams occur in the REM stages. Our Environment Outside SleepHave you ever had a dream where someone next door is playing music, and the music is conveniently woven into your dream? This is your body trying to lessen the chances of you awakening while it is repairing itself. However, sleep deprived people go into much deeper sleep, and may not detect such noises. The overriding point here is, that sleep is essential to the body, and that there are compensations made to our usual behaviour (like paralysis) that enables our body to do what is required for itself. Sleep TroublesThe older we get, the less sleep we require. Teenagers buck the trends in needing the most sleep of us all, due to the growth spurt occurring at puberty that involves a larger turnover of materials and energy.
Certain drugs are available to induce sleeping, but most are addictive and require controlled and responsible use. The next page looks at the works of famous past neurologists like Carl Gustav Jung and Sigmund Freud, who both actively pursued the way in which we dream as a career in neurology. |
Sigmund Freud and Carl Gustav Jung
- Human Neurology
Sigmund FreudSigmund Freud was a famous Austrian neurologist (1856 - 1939), who stated that dreams were the manifestation of the unconscious. Himself and another neurologist, Carl Gustav Jung (1875 - 1961), believed that conscious behaviour derived from unconscious instinct which exists in all of us. These unconscious thoughts were linked to suppressed sexual desires. Freud identified three key stages in the life cycle where the child's tendency to focus on sexual areas of the body changes over time.
Freud argued that in these stages of unconscious repression, male children are attracted to their mother and become instinctively aggressive towards the father. The father reciprocally injects fear into the child by his male superiority, thus insinuating an essence of competition and games theory. Either way, the prime fact is that the child must grow to become sexually active and mature. Differences Between Jung and FreudJung believed that a persons' brain consisted of the forgotten conscious and a cluster of memories of past experiences. He came to this hypothesis by studying humans suffering a mental disorder, who had hallucinations that were not a past recollection, thus Jung deduced there was another component of the brain adding to this illusion, i.e. the unconscious. Freud on the other hand believed that the brain was divided into three parts
Essentially, this method of thinking, and approaching the brain from a self-realizing approach, neurology has been able to develop since these initial theories by Jung and Freud. It also paved advance in psychiatry, and methods of psycho therapy to combat mental disorders, which are investigated upon in the next page. |
Psychiatry & Mental Disorders
- Human Neurology
The Definition of MadWhen someone says 'mental disorder' many people associate it with madness. This is truly not the case. There are many states of mental disorder where the sufferer is not clinically insane. Madness essentially means psychosis, being out of touch of reality and not being capable of rational and controlled thought. A person in psychosis may have irrational delusions and hallucinations that illustrate this imbalance in conscious and unconscious mind. SchizophreniaSchizophrenia can effect mind and personality. In severe cases, the sufferer believes that 'something' is in control of them, and that they have lost control of themselves. Affective Mood Disorder
Obsessive & Compulsive DisorderA mental disorder where the sufferer must undergo meticulous rituals to live their normal lives, such as excessive washing of their skin and hair. If the sufferer cannot do this, anxiety kicks in as a "withdrawal symptom" until they allow themselves to repeat the ritual once again. PhobiasA preconception about a given situation or object, such as a fear of snakes or being in high places. A huge diversity of phobias have been discovered by psychologists. Depressive NeurosisThe classic case of depression where depression is the primary emotion in the sufferer, resulting in a lack of motivation and self-esteem to be functional in society and to themselves. Physical DiseaseNot only can the way the brain works be affected by disorders, the physical components of the brain can also be infected by pathogens. Dementia is such a physical disease, where the long term memory of the sufferer is broken down due to the physical components of the brain and nervous synapses degrading over time. Drugs for Mental DisordersA wide range of drugs are now available for those suffering mental disorders, though many people face a psychological barrier when it comes to taking medication to cure their 'soul'. Many of the drugs used prove addictive which in turn can also lead to further psychiatric problems. However, psychotherapy is an alternative communicative treatment designed to get the patient to understand themselves better. This can be combined with drugtherapy, and eventually develop the patients' self realisation into a moreproductive and positive state. Medicinal neurology is a fairly new area of medicine. The next page investigates perception and two people can interpret the same thing differently. |
Human Perception - Neurology
- Human Neurology
A better understanding of human perception
unlocks the key to how the mind works, an
advantage when working with people with mental
disorders.
Visual PerceptionThe below diagram is an illustration as to how we all perceive things in our own way, as suggested by the theories of Jung and Freud.
What do you see? Some of you may see 2 green faces, other may see a white chalice. This all depends on your initial perception of the diagram. You may find that when you look again, you may see the alternate picture within the diagram. The retina is responsible for interpreting visual stimuli such as this, where it picks up photons of light via the 130 000 000 rods and cones situated on it. In pre-modern times it was considered that visual perception simply encompassed what was seen by the eye on the outside. This external stimuli would in turn produce a perception in the brain caused by the stimulus. However this is not the case. Modern medicine now knows that information from the eye is simply a physiological process that does not actually process the signals it receives. This job is left to the brain. The senses simply act as a messenger to a particular stimulus that is seen, the brain is the place where external stimuli is actually perceived. Spatial AwarenessThe environment we live in is 3 dimensional, thus needs a 3 dimensional approach to understand it. Therefore height, width and depth must be measured by the eyes This is possible by the way the eyes are situated on the head. Positioned either side of the nose, the right eye picks up vision on the left hemisphere and the left eye picks up vision in the right hemisphere. The images picked up by the eyes are projected upside down on each of the eyes retina. This in turn will be perceived the right way up by the brain, which will interpret the three dimensional values of the external environment at a very fast and effective rate IllusionsIt is possible for the physiological state of the brain to deviate from the norm and trigger of a mental disorder. Illusions are a symptom of such mental disorders. However it is also possible to trick the senses of a perfectly functional healthy brain. Illusions, such as the mirages that appear in the desert are caused by trickery of the sense, leading us to believe there is something out there when this is not the case. More information on illusions and mind trickery are looked upon in the next page |
Neurology of Illusions
- Human Neurology
As mentioned in the previous page looking at
perception, illusions can be caused by mental
disorders or misreading of the sensory data
obtained from the external environment. For now
we will look at the latter.
Visual Illusions
Auditory IllusionsOne of the most famous of these is the Doppler Effect, where a noise situated close to you has a higher pitch of sound to that of a sound further away. This is the case if you should and get an echo, your voice will always sound more deeper in the echo when it is not. This is effectively an illusion. The Study of IllusionsAs mentioned previously, the study of illusions in sufferers of a mental disorder provide a key into a deeper understand of what is going on in their mind. This is also the case of a healthy brain, where the study of illusions can work out the parameters at which it compensates for its own lack of ability It is worth noting that the trial and error the sensory organs function have, they are as just as foolproof as any other conscious human thought. The chances of your brain not being able to guess the spatial distance of a fuzzy moving object is the same lack in ability that people have in typing an error free document In this sense, illusions is studying the perceptions and sensory data obtained from situations where human error prevents us from seeing the real deal. Another interesting fact is that the retina is read by the brain every 0.1 seconds, meaning that you are not actually seeing anything in the present, but something that just happened a fraction of a second ago. |
Central Nervous System
|
Peripheral Nervous System
|
Autonomic Nervous System
|
Functions of the Nervous System
The complex activities of the body are controlled jointly by the Endocrine and the Nervous systems. As opposed to the Endocrine system the Nervous system has a more or less instant effect on the body via a complex network of nerves and control centres. The Central Nervous System (CNS) includes the brain and spinal cord, while Peripheral Nervous System (PNS) includes nerves connected to the spinal cord. The nervous system can be further divided into sub-systems, all of which are composed of neurons and connective tissue: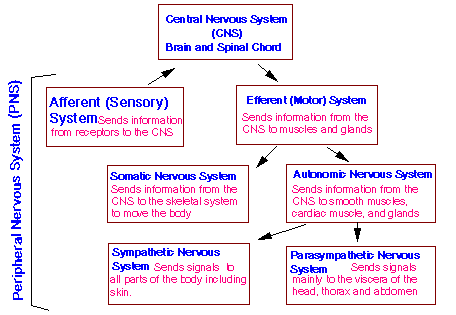
About Neurons
Neurons are specialised cells of the nervous system, they vary greatly in appearance and length, but contain a similar structure:- Axons are long nerve processes which carry nerve impulses from the Soma to other neurons, they vary in length but can become almost as long as half of the human body.
- The soma (body) of the neuron contains the nucleus which acts as the cell's control centre, these contain many small neurofibrils which project from the nucleus into the dendrites.
- Dendrites are short, thick processes which branch out of the soma in a tree like manor. They conduct nerve impulses to the soma.
The three categories of neurons:
- Afferent (Sensory) Neurons have the dendrites connected to receptors such as the eyes, ears etc. These receptors change the information they receive into electrical impulses that are transmitted to other neurons. In sensory neurons the axons are connected to other neurons.
- Efferent (Motor) Neurons have the dendrites connected to other neurons, the axons are connected to effectors. Effectors are either glands or a muscle cell that is the receiving end of the nerve impulse. The nerve, when excited will cause the effector to react (move, contract, or secrete etc).
- Internuncial Neurons have both the dendrites and the axons are connected to other neurons. They are sometimes referred to as connector neurons. Internuncial neurons are found throughout the body, but especially in the spinal cord and brain.
Properties and characteristics of Neurons:
- Normally the electrical impulses (messages) travel through a neuron in only one direction.
- The axon may be surrounded by a 'coat' of lipids (fats) and proteins known as the myelin sheath which acts as an insulator.
- Neurons are specialist cells that have lost the ability to reproduce themselves. Once the soma of a neuron has died the entire neuron dies, and can never be replaced.
- Repair of damaged neurons only occurs in myelinated neurons.
- white matter are coloured by myelin, consisting of many neurons supported by neuroglia.
- grey matter is soma and dendrites or bundles of unmyelinated axons and neuralgia.
Nerves, Neuroglia, and Ganglia
A nerve is a bundle of fibres (axons and/or dendrites) outside the CNS.Neuroglia are cells of the nervous system that help protect and support it.
Ganglia are groups of nerve cell bodies lying outside the CNS.
The Spinal Chord
A spinal tract is a bundle of fibres in the CNS that travel long distances up or down the spinal chord. Ascending tracts carry impulses up the chord to the brain, while descending tracts carry impulses down the chord from the brain. Tracts run along the spinal canal inside the protective spinal column, conveying sensory and motor (movement ) information to and from the brain. Spinal meninges are tough tubes of tissue which protect the chord.
The Brian
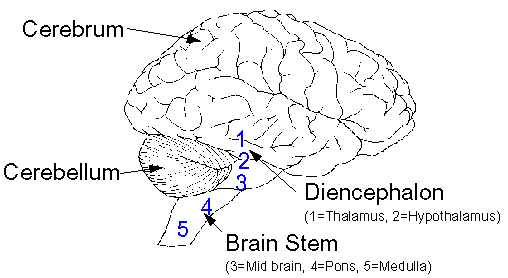
The brain is highly complex, it contains about 1000 billion neurons, and weighs about 3 lbs in adults.
There are four main areas of the brain:
- The brain stem is at the base of the brain where it joins the spinal chord (contains the medulla, pons, and mid brain)
- The diencephalon is above the brain stem (contains the thalamus and hypothalamus)
- The cerebrum is above the diencephalon and forms the majority of the brain
- The cerebellum is the lower back of the brain
The brain has two hemispheres , there are functional differences, for example the left had side of the brain controls the right hand side of the body and visa versa (lateralisation).
Neurotransmitters are substances which excite or inhibit the neurons of the brain, facilitating communication between brain cells. These include endorphins, neuropeptides.
Cerebrospinal fluid circulates around the brain and spinal tracts to provide protection in addition to that provided by the meninges and protective bones of the spine and skull. A lumbar puncture (spinal tap) is where a needle is placed between the vertebra in the lower back. A sample of cerebrospinal fluid might be taken to see if cancerous cells have entered the CNS, or chemotherapy might be administrated to prevent or combat CNS involvement.
The Sensory Systems
A receptor or sense organ picks up stimulus and converts it into a nerve impulse. This impulse is then conducted along a neural pathway to the brain, where the signal is converted into a sensation. There are various receptors:- Cutaneous (skin) senses. The skin contains specialist receptors for touch, pressure, vibration, hot, cold, and pain.
- Proprioceptive (muscle) sensations inform us of the activities and current posture of the muscles.
- Integrative sensations are not well defined but include memory, sleep, emotions etc.
- Olfactory sensations (smell). Olfactory neurons have dendrites that are connected to fine hairs in the nose that react to odours.
- Gustatory sensations (taste) there are about 2000 taste buds, mostly on the tongue and a few in the throat. Taste buds contain gustatory cells which contain sensitive hair like processes.
- Ophthalmic sensations (sight). The retina of the eye converts light into nerve impulses which are transmitted to the optic nerve. Retinoblastoma is a rare tumour in the cells of the retina.
- Auditory senses (hearing). Sound waves cause fine hairs in the inner ear to vibrate generating nerve impulses.
- Equilibrium (sense of balance) the ear also contains receptors that give a sense of static equilibrium (position of the head) and dynamic equilibrium (sudden movements).
The Autonomic Nervous system (ANS)
The nerves of the ANS activate the involuntary smooth muscles, cardiac muscles, and some glands.
Roots, suffixes, and prefixes
| component | meaning | example |
| ASTRO- | star | |
| astrocyte = star shaped brain cell. | ||
| CRANI- | skull | |
| cranial radiation = radiation to the head. | ||
| CEPHAL- | head | |
| encephal = the brain, en(in) cephal (the head). | ||
| MENING- | membrane | |
| meningitis = inflammation of the membranes of the spinal chord. | ||
| NEUR- | nerve | |
| neuroblast = an immature nerve cell. | ||
| VENTRICULO- | cavity | |
| ventricles are small cavities in the brain & spinal cord. Ventriculscopy = examination of ventricles. | ||
| -MALACIA | softening | |
| neuromalacia = morbid softening of the nerves. | ||
| -GRAM | record | |
| electroencephalogram (EEG) = brain scan. |
Cancer Focus
- Overview of CNS Tumours
- Adult CNS Tumours
- Childhood CNS Tumours
- Cancers of the Eye
- Retinoblastoma
- Intraocular Melanoma
- Neuroblastoma
- Related Abbreviations and Acronyms
- Childhood CNS Tumours
- Childhood Brain tumours are the second most common type of
childhood cancer. They are however a diverse group of different
types of tumours. Classification of brain tumours is based on both
histopathology and location in the brain. For example,
undifferentiated neuroectodermal tumours of the cerebellum are
referred to as medulloblastomas, while tumours with similar
histology in the pineal region would be diagnosed as pineoblastomas.
Patients may present with headaches, drowsiness, weakness, or
vomiting caused by the pressure inside the skull caused by the
growing tumour.
Medulloblastoma is nearly always found in children or young adults, 80% are found in children aged under 15. It can spread from the medulla (part of the brain stem) to the spine or to other parts of the body. Prognosis will depend on the child's age, how much of the tumour remains following surgery, and whether the cancer has metastasised.
Cerebellar astrocytoma arise in brain cells called astrocytes. Cerebellar astrocytoma is usually low grade (slow growing and non metastatic cells), while Cerebral astrocytoma can be malignant.
Brainstem gliomas are tumours arising in the mid brain, pons or medulla. They may grow rapidly or slowly, depending on the grade of the tumour, but overall have a less favourable prognosis compared to other tumours such as Cerebellar astrocytoma.
Other brain tumours include: Primitive neuroectodermal tumour (PNET), craniopharyngioma, intracranial germ cell tumour, pineal parenchymal tumour, and optic tract glioma.
- Retinoblastoma
- Retinoblastoma is a rare tumour of the eye which develops in the cells of the retina, most patients are under 5 years old. Sometimes only one eye is affected (unilateral-retinoblastoma ), but in about two fifths of patients both eyes have the disease (bilateral-retinoblastoma ). Some cases are known to be hereditary.
-
 Internet Resources for
Retinoblastoma
Internet Resources for
Retinoblastoma
- Intraocular Melanoma
- Intraocular melanoma is a rare cancer, in which malignant cells are found in the uvea (this is the part of the eye which contains the iris and other tissues). The uvea contains melanocytes which are cells that contain colour, intraocular melanoma occurs when these cells become cancerous.
-
 Internet Resources for
IntraOcular Melanoma
Internet Resources for
IntraOcular Melanoma
- Neuroblastoma
- Neuroblastoma occurs most often in babies, very young children. It is a disease in which cancer cells are found in certain nerve cells in the body, it originates in the adrenal medulla or other sites of sympathetic nervous system tissue. The most common site is the abdomen, either in the adrenal glands or around the spinal cord. The majority of patients present with metastatic disease. Age and stage are the main prognostic factors. Patients aged under one year at diagnosis have a more favourable prognosis. Stage 4S are a special group of patients aged under one year whose neuroblastoma may undergo spontaneous regression (tumour disappears without treatment). Also patients aged under one a higher proportion of low stage patients compared to older patients. There is an excess of males compared to females, there are a higher proportion of males in patients with less favourable sites and stage.
-
 Internet Resources for
Neuroblastoma
Internet Resources for
Neuroblastoma
Related Abbreviations and Acronyms:
-
ABTA American Brain Tumour Association BAER Brainstem Auditory Evoked Responce CNS Central nervous system - the brain and spine CSF Cerebro spinal fluid EANO European Association for NeuroOncology EEG Electroencephalogram - brain scan ENSG European Neuroblastoma Study Group INFA International Neurofibromatosis Association INSS International Neuroblastoma Staging System LP Lumbar puncture NNFF National Neurofibromatosis Foundation (USA) NSE Neuron-Specific Enolase - a neural marker PNET Primitive neuroectodermal tumour Context: CNS tumours PNS Peripheral nervous system - nervous system outside the brain and spine.